Patients with lower back pain prescribed skeletal muscle relaxants in addition to NSAIDs report the same outcomes as placebo plus NSAIDs, new research shows.
“Combining a skeletal muscle relaxant with an NSAID does not confer any additional benefit,” Lorena Abril, MD, Montefiore Medical Center, New York City, told Medscape Medical News in an interview following her abstract presentation at the annual American College of Emergency Physicians (ACEP) online congress.
There are 2.6 million visits to emergency departments in the US annually for lower back pain, Abril said in her presentation. One third of patients report persistent back pain and 1 in 5 report limitations in activity, she explained.
Acute lower back pain “is generally considered a condition with a favorable prognosis, regardless of treatment,” Abril said. The current American College of Physicians guideline for noninvasive treatment of acute, subacute and chronic low back pain (LBP), published in 2017, recommends that if a pharmacologic treatment is desired, NSAIDs or skeletal muscle relaxants (SMRs) should be used. But “no pharmacological treatment…has been shown to provide a moderate or large effect on pain or function in patients with acute low back pain,” Abril said.
To see if SMRs improved prognosis at 1 week after discharge from hospital, investigators enrolled 889 patients with lower back pain from the emergency department into a randomized, placebo-controlled trial. Patient mean age was 39; 56% were female, 44% male.
All patients completed the Roland-Morris Disability Questionnaire (RMDQ) before leaving the hospital and again after 1 week follow-up. Abril explained that RMDQ has been shown to correlate well with other tests that measure physical disability, including the Quebec Back Pain Disability Scale, the Oswestry Low Back Disability Questionnaire (ODI), and the physical subscales of the Sickness Impact Profile, among others.
In the initial RMDQ performed with patients, the median score overall was 18, (ranging from 16 to 22) on a 24-point scale.
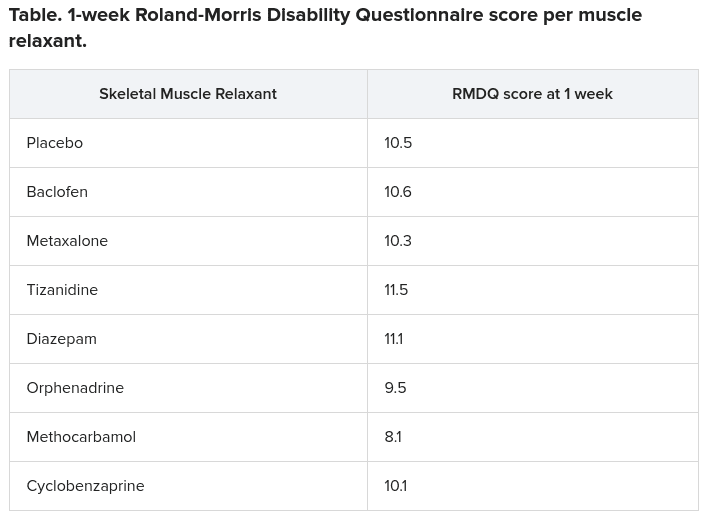
On discharge, patients were prescribed 1 of 7 skeletal muscle relaxants (SKMs — baclofen, metaxalone, tizanidine, diazepam, orphenadrine, methocarbamol, or cyclobenzaprine) or placebo in addition to an NSAID such as naproxen or ibuprofen.
At 1-week follow-up, 858 (96.5%) patients completed a second RMDQ. Although all scores were improved, researchers found no significant difference in RMDQ scores between patients receiving placebo or any of the SKMs. “The between-group differences failed to achieve clinical differences. In fact, placebo was superior to methocarbamol with a mean difference of 2.4,” said Abril.
“As investigators continue to research the appropriate use of muscle relaxants as part of a multimodal approach to low back pain in the ED, the evidence continues to show these medications have a limited role,” Alexis LaPietra, DO, of St. Joseph’s University Medical Center, Paterson, New Jersey, told Medscape Medical News. LaPietra was not involved in the study.
“Even when they analyzed subtle differences in sex, age, and baseline severity, they had consistent findings that none of the traditionally used muscle relaxants add much benefit to the recommended analgesic regimen,” LaPietra added. “More pain research is need to equip clinicians with up-to-date, evidence-based concepts to help manage the complex, disabling, but very common complaint of low back pain in the ED.”
Abril said her team is considering studies of other medications for patients presenting to the ED. Because poor pain and functional outcomes persist beyond the hospital visit for patients with acute musculoskeletal LBP, and because research shows topical NSAIDS might be more effective than oral NSAIDS, “we are currently designing a clinical trial to test the effectiveness of topical diclofenac in patients presenting to the ED primarily for management of nontraumatic, nonradicular musculoskeletal LBP,” she said.
Nonpharmacologic treatment, including superficial heat, massage, acupuncture, or spinal manipulation, is initially recommended for most patients with acute or subacute low back pain, Abril said. “This is an interesting and important topic for future research, starting with the need for validated, properly described and standardized methods of measuring and reporting clinical outcomes, which is a major limitation of the literature.”
“Finding a solution,” she added, “is a challenge that we hope can be solved soon.”
What do you prescribe for your patients with back pain? Tell us in the comments.
American College of Emergency Physicians (ACEP) 2020: Abstract 15. Presented October 24, 2020.
Ingrid Hein is a freelance health and technology reporter based in Hudson, Quebec.


Recent Comments